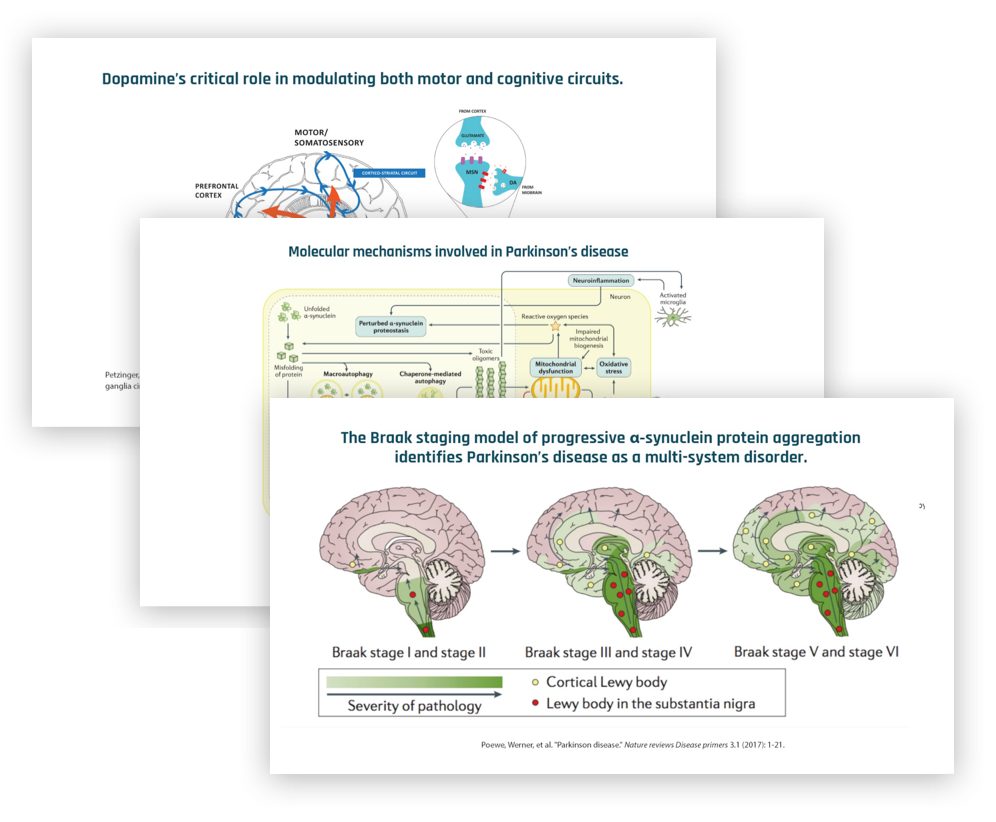
By becoming a member of FoundMyFitness premium, you'll receive the Science Digest every-other-week covering the latest in my exploration of recent science and the emerging story of better living — through deeper understandings of biology.

- Ketogenic diet, by replacing glucose with ketones as an energy source, lessens alcohol cravings among people with alcohol use disorders.
- Omega-3 fatty acids reduce the risk of cardiovascular disease-related death by up to 23 percent, especially in people with high triglyceride levels.
- Women see a 24 percent drop in premature death risk with just 140 minutes of weekly activity – half the time men need for similar benefits.
- Aging undermines the brain's capacity for maintaining working memory, with subtle declines in neuron activity and connectivity in the prefrontal cortex.
Plant-based meat substitutes are made from non-meat sources, such as legumes or wheat gluten. They typically mimic the sensory profile of meat products and are popular among those wishing to reduce their animal protein intake for ethical or health reasons. A recent study found that plant-based meat substitutes did not benefit cardiometabolic health in people at risk for type 2 diabetes.
The study involved 82 adults at risk for type 2 diabetes. Half of the participants ate an animal-based diet, while the others swapped out their usual animal-based foods for plant-based meat substitutes. Researchers assessed their blood lipids (triglycerides, LDL, HDL, and total cholesterol), glycemic control, insulin sensitivity, and blood pressure before and after the eight-week intervention.
They found that participants who ate the plant-based meat substitutes had higher fiber, sodium, and potassium intake than those who ate animal meat. Their blood lipids showed little improvement, but their diastolic blood pressure decreased, and their insulin sensitivity increased. However, those who ate the animal meat diet had better glycemic control than those on the plant-based diet.
These findings suggest that plant-based meat substitutes don’t improve cardiometabolic health in people at risk for type 2 diabetes. However, robust evidence demonstrates that high-intensity interval training (HIIT) profoundly affects cardiometabolic health. Learn more in this episode featuring Dr. Martin Gibala.
Polyfluoroalkyl substances, or PFAS, are synthetic compounds used in food packaging, household products, and drinking water. PFAS aren’t excreted in bodily fluids like sweat or urine; instead, they persist in the body indefinitely and are often referred to as “forever chemicals.” A recent study found that seafood – including fish and shellfish – contains high PFAS levels.
Researchers asked more than 1,800 people living in the northeastern U.S. about the amount and types of seafood they ate. Then, they measured PFAS levels in fish, lobster, shrimp, and scallops purchased from a market in that area.
They found that the participants were regular seafood consumers, with adults consuming approximately 34 grams daily and children consuming 5 grams – slightly higher than national averages. They also found that the fish contained less than 1 nanogram per gram (ng/g) of PFAS; the shrimp contained 1.74 ng/g, and the lobster contained 3.30 ng/g. These levels may pose health concerns among high seafood consumers.
These findings suggest that seafood is an abundant source of PFAS. Future research may illuminate the benefits and risks of consuming seafood. Exposure to PFAS has been linked to various health issues, including increased cholesterol levels, changes in liver function, and impaired immune function. Some studies suggest a potential association between PFAS exposure and increased risks of certain cancers and reproductive problems
Statins are among the most widely prescribed drugs in the U.S., with more than 92 million users reported in 2018. Although the drugs are generally effective, nearly 22 percent of statin users with cardiovascular disease will experience a major adverse cardiovascular event within five years of drug initiation – a phenomenon known as “residual risk.” Findings from a recent meta-analysis indicate that combined statin-omega-3 therapy markedly reduces the risk of major adverse cardiovascular events and improves lipid and inflammatory markers.
Researchers analyzed the findings of 14 randomized controlled trials involving more than 40,000 participants. The trials investigated links between statin use, omega-3s, and the risk of cardiovascular disease and related death. Omega-3 doses varied, ranging from 930 milligrams to 4,000 milligrams daily. However, most studies provided a dose of 1,800 milligrams daily.
They found that combined statin-omega-3 therapy reduced the residual risk of experiencing myocardial infarction (heart attack) by 28 percent, a major adverse cardiovascular event by 15 percent, angina (chest pain) by 25 percent, and hospitalization for angina by 25 percent. Those receiving the combined treatment also experienced decreased cholesterol, triglycerides, and hsCRP (a marker of inflammation). However, the combined therapy did not reduce the residual risk of fatal and non-fatal stroke, coronary revascularization, and cardiovascular disease-related death.
These findings suggest that combined statin-omega-3 therapy reduces the residual cardiovascular risks associated with statin therapy alone. Learn more about statins in this episode featuring Dr. Peter Attia.